
Is Diabetes Forever
Is type 2 diabetes forever? It’s what type 2 diabetics are told from the time they are diagnosed. For too many, the answer is yes. The answer can also be …
Read More
Is type 2 diabetes forever? It’s what type 2 diabetics are told from the time they are diagnosed. For too many, the answer is yes. The answer can also be …
Read More
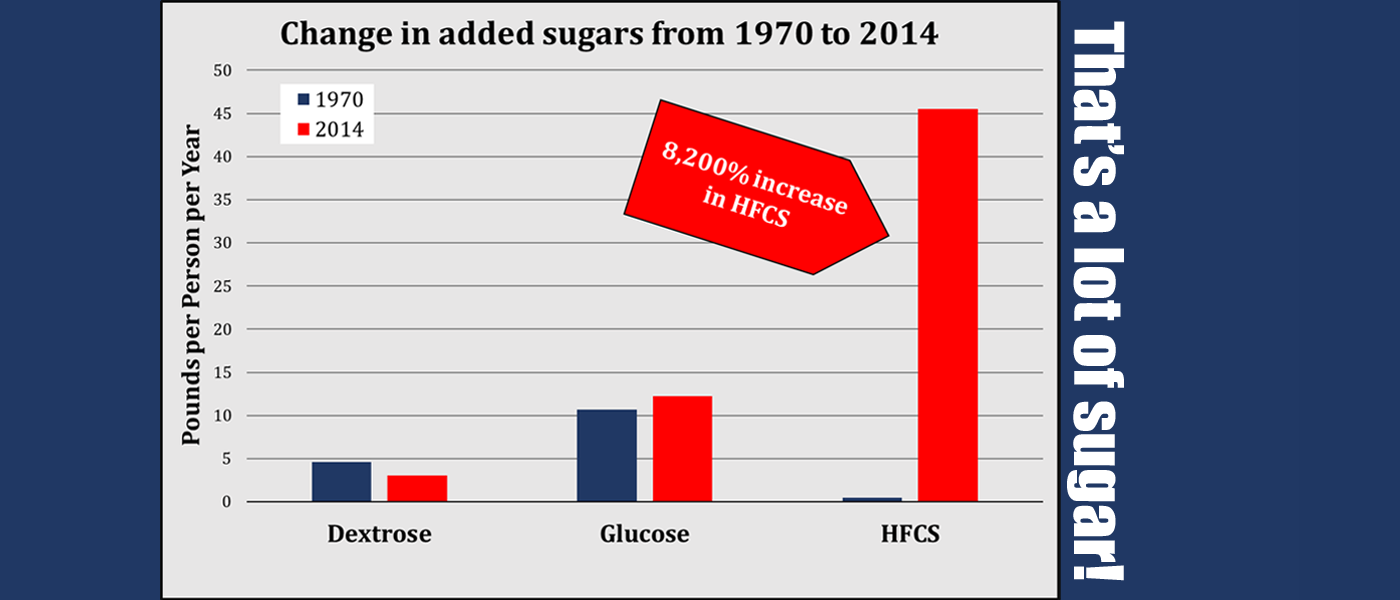
Would you like to know why our chronic disease problem is so bad? Look no further than this! The USDA recently published “U.S. Trends in Food Availability and a Dietary …
Read More
That’s it – 2 minutes. After a great weekend and time spent on Sunday prepping for Monday, I was ready. Around 5:30am, this is sitting at the top of my …
Read More
Implanting sponges in fat tissue? Things are getting crazy! This report suggests that implanting sponges into the fat tissue of type 2 diabetics may be a helpful process, as a …
Read More
Type 2 diabetes is a significant burden on our healthcare system and likely worse than current estimates. Despite this, the real issue is what will happen in the next 10, …
Read More
3 Snacks Type 2 Diabetics need to keep with them at ALL times! No blood sugar impact snacks Most type 2 diabetics struggle with controlling their blood sugar. Since almost …
Read MoreThank you for viewing our webinar! Listed below are links where you can download the files discussed during the webinar – the exercise tip sheet and the Module 1 Guide. …
Read MoreControlling blood sugar is not enough! A recently published article confirms what many other articles have shown: For type 2 diabetics, controlling blood sugar does not reduce the risk of …
Read More